Compounds that do not allow blood to clot are called anticoagulants. These include drugs such as heparin and coumarin. Drugs that dissolve pre-formed clot including streptokinase are not referred to as anticoagulants.
Anticoagulants are usually administered to patients with myocardial infarction, venous thrombosis, peripheral arterial emboli and pulmonary emboli. They have been used to prevent transient ischemic attacks and to reduce the risk of recurrent myocardial infarction.
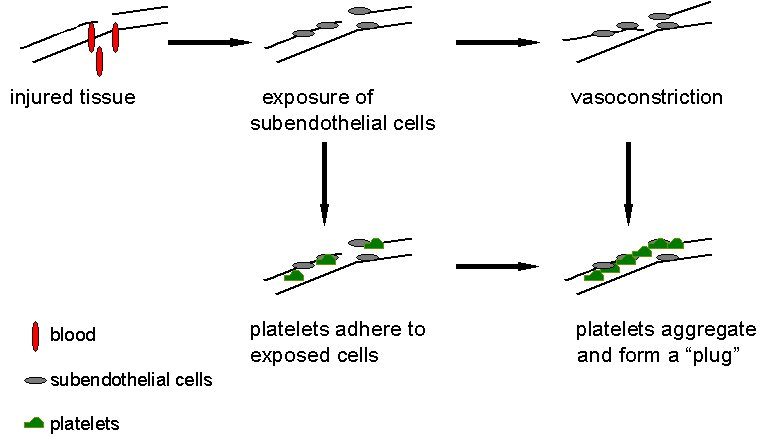
The circulatory system has to be self-sealing, otherwise continued blood loss from even the smallest injury would be life threatening. Normally, all but the most catastrophic bleeding is rapidly stopped, a process known as hemostasis. This process occurs through a progression of several steps.
Hemostasis is a combination of events that occur due to physical and chemical forces. The initial steps lead to a reduction in the blood flow due to the formation of a cellular plug. The later steps utilize chemical energy to form a blood clot, medically known as thrombus.
The Physical Process

The aggregating platelets and the damaged tissue initiate the biochemical process of blood clotting or coagulation, the body's major defense against blood loss.
A blood clot forms as a result of concerted action of some 20 different substances, most of which are plasma glycoproteins (Table).
| Coagulation Factors | ||
| Factor | Name | Plasma half-life (h) |
| I | Fibrinogen | 72 - 96 |
| II | Prothrombin | 60 |
| III | Tissue Factor or thromboplastin | -- |
| IV | Ca++ | -- |
| V | Proaccelerin | 15 |
| VII | Proconvertin | 5 |
| VIII | Antihemophilic A factor | 10 |
| IX | Antihemophilic B factor or Christmas factor | 25 |
| X | Stuart or Stuart-Prower factor | 40 |
| XI | Plasma thomboplastin antecedent | 45-65 |
| XII | Hageman factor, contact factor | 60 |
| XIII | Fibrin stabilizing factor | 150 |
| Prekallikrein factor | -- | |
| High-molecular-weight kininogen | 156 | |
The phenomenon of blood coagulation is traditionally distinguished into two pathways. These pathways are the intrinsic and the extrinsic pathways (Figure below). The intrinsic pathway is defined as a cascade that utilizes only factors that are soluble in the plasma, whereas the extrinsic pathway consists of some factors that are insoluble in the plasma, e.g., membrane-bound factors (factor VII). However, the boundary differentiating these two is becoming more and more blurred.
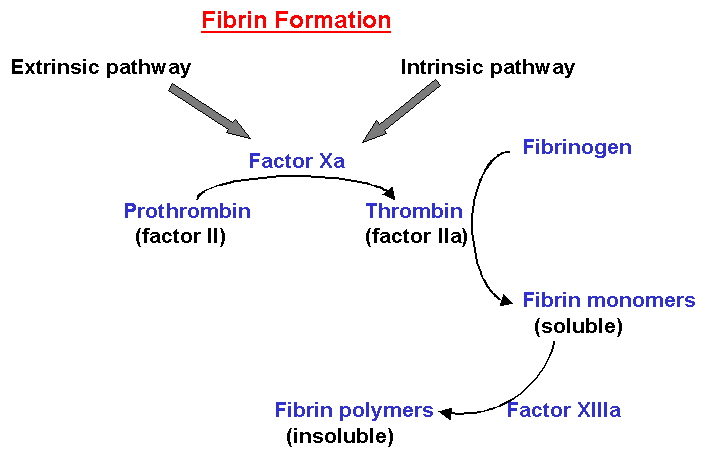
The characteristic feature of the coagulation pathway is that upon activation the individual glycoprotein serves as a enzyme to convert the zymogen form of the succeeding glycoprotein to its protease form only in the presence of Ca+2 cations and on an appropriate phospholipid membrane. The activated forms of the glycoproteins are identified by symbol 'a'.
Both the intrinsic and the extrinsic coagulation pathways proceed through a common pathway by forming activated factor X. Prothrombin is cleaved at two sites by factor Xa to yied thrombin (To see a structure of thrombin molecule click here). Ten g-carboxyglutamic acid residues are located on the N-terminal end of the prothrombin molecule. Vitamin K is required in the liver biosynthesis of the prothrombin g-carboxyglutamic groups by participating in the carboxylation of the g-carbon of glutamic acid. These carboxy groups are required for binding calcium to prothrombin, which induce a conformation change in prothrombin enabling it to bindi to co-factors on the phospholipid surfaces during its conversion to thrombin by factor Xa, factor V, and platelet phospholipids in the presence of calcium.
Thrombin, in turn, cleaves fibrinogen. Fibrinogen comprises 2-3% of plasma protein. Thrombin specifically cleaves the Arg-X (X is mostly Gly) peptide bond in fibrinogen to form soluble fibrin monomers. These monomers spontaneously aggregate to form a polymeric structure called "soft clot". This polymer is rapidly converted to a more stable "hard clot" by the covalent cross-linking of neighboring fibrin molecules in a reaction catalyzed by fibrin-stabilizing factor (FSF or XIIIa).
The multilevel cascade of blood clotting system permits enormous amplification of its triggering signals. Moving down the extrinsic pathway, for example, proconvertin (VII), Stuart factor (X), prothrombin, and fibrinogen are present in plasma in concentrations of <1, 8, 150, and ~4000 mg.mL-1, respectively. Thus a small signal is very quickly amplified to bring about effective hemostatic control.
On the other hand, clotting must be very strictly regulated because even one inappropriate clot can have fatal consequences. Indeed, blood clots are the leading cause of strokes and heart attack, the two major causes of human death.
Endogenous Inhibitors of Clotting
Thrombin plays a pivotal role in blood coagulation and Nature has designed several serine protease inhibitors (SERPINS) to regulate the its activity. These include antithrombin (major), heparin cofactor II, a2-macroglobulin, and a1-proteinase inhibitor.
Antithrombin is present in the plasma in significant concentrations (~2-3 mM). Antithrombin primarily neutralizes factor Xa and thrombin, in addition to inhibiting most active serine proteases of the clotting system. (To view a structure of antithrombin click here.)
Protein C is another plasma protein that limits clotting by being activated by thrombin to proteolytically inactivate proaccelerin (V) and antihemophilic factor (VIII).
Thrombomodulin, a cell membrane bound glycoprotein lining the vascular endothelium, specifically binds thrombin so as to convert it to a form with decreased ability to catalyze clot formation but with a >1,000-fold increased capacity to activate protein C.
Exogenous Inhibitors of Clotting
The control of clotting is a major medical concern. Several inhibitors have been developed with different mechanisms of anticoagulant action. These include the heparins, the coumarins, and the 1,3-indanediones.
[top] [session home] [home] [department of medicinal chemistry] [school of pharmacy]
©2000 VCU School of Pharmacy
Revised: January 5, 2000
Questions or Comments : Dr. Umesh R. Desai